
Not just isolated case reports
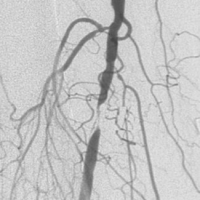
The signal was clinically visible: aOR 1.25 for MI, 1.42 for stroke, and 1.28 for a composite cardiovascular outcome.
Machine Generated Science • ISSN 3054-3991
DOI: 10.62487/saimsara242a8e10

The signal was clinically visible: aOR 1.25 for MI, 1.42 for stroke, and 1.28 for a composite cardiovascular outcome.

Another prescribed-cannabis cohort in chronic pain found higher new-onset arrhythmia risk within 180 days.
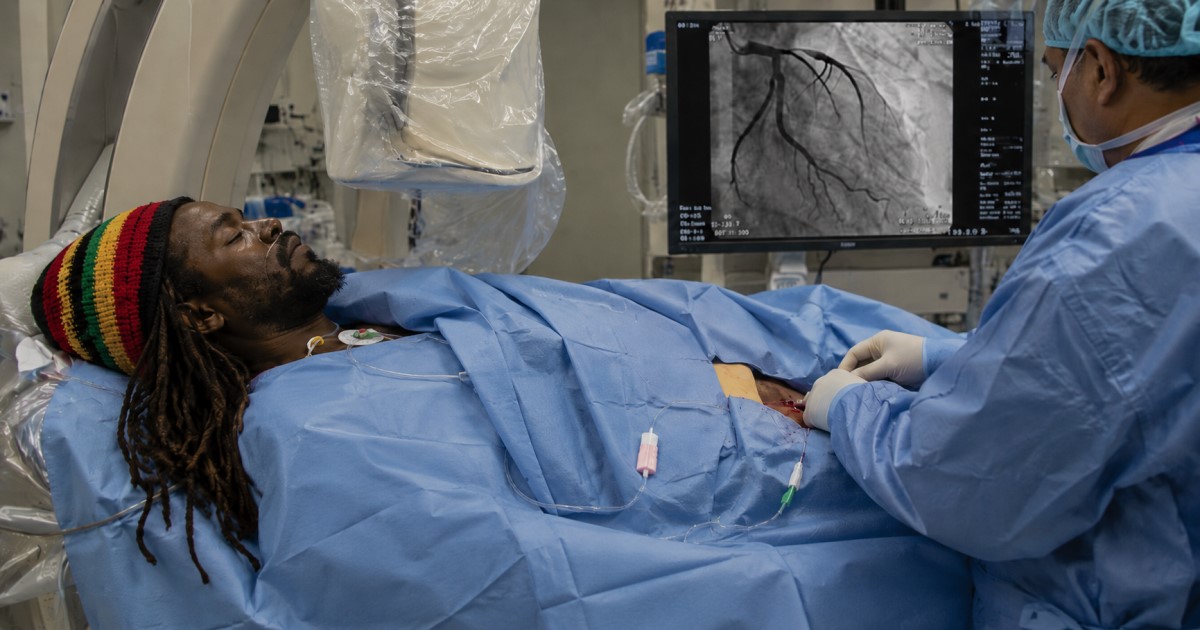
That is the clinically important gap: cannabis risk depends on dose, timing, product type, endpoint, and patient vulnerability.
Unlock the full evidence map
The full evidence review, including the Introduction, Methods, Results, Discussion, Conclusion, figures, and complete reference index, opens after purchase or sign-in. The Evidence Object JSON is a separate machine-readable evidence product: a concentrated synthesis of results, topic-level evidence, and discussion across original and non-original studies. It can be directly input into your LLM, agent, or RAG workflow.