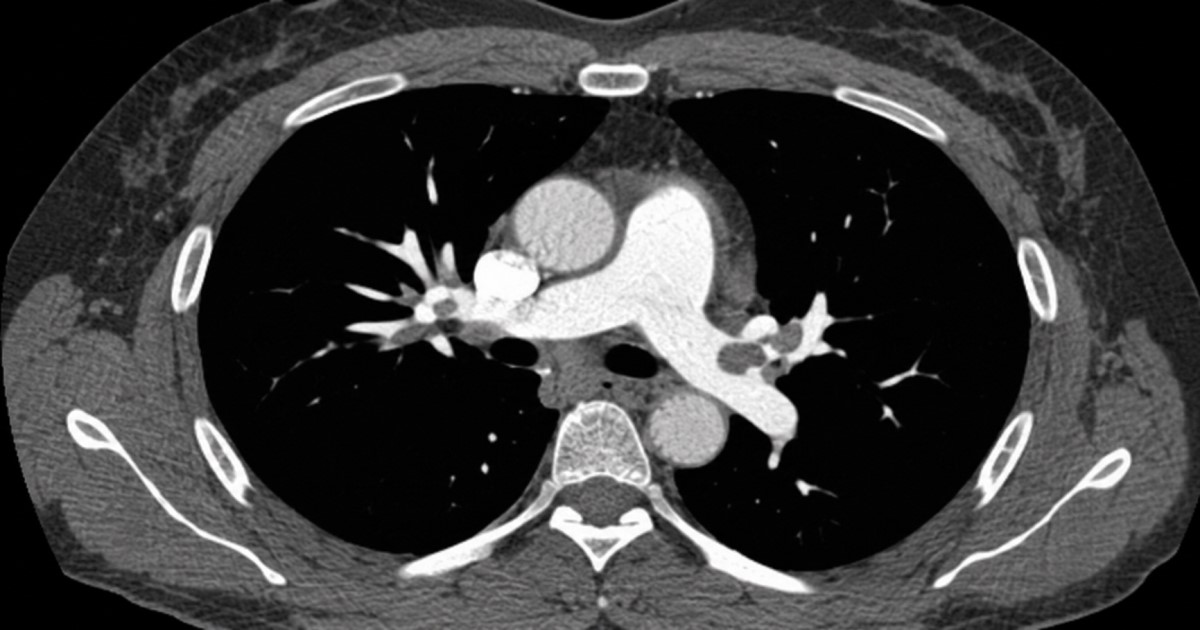
A knee-vein lesion can present in the lungs
This makes PVA clinically important far beyond a local finding behind the knee.
Machine Generated Science • ISSN 3054-3991
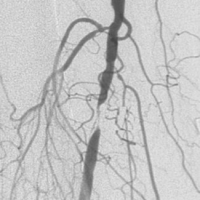
DOI: 10.62487/saimsaraee3198be

This makes PVA clinically important far beyond a local finding behind the knee.
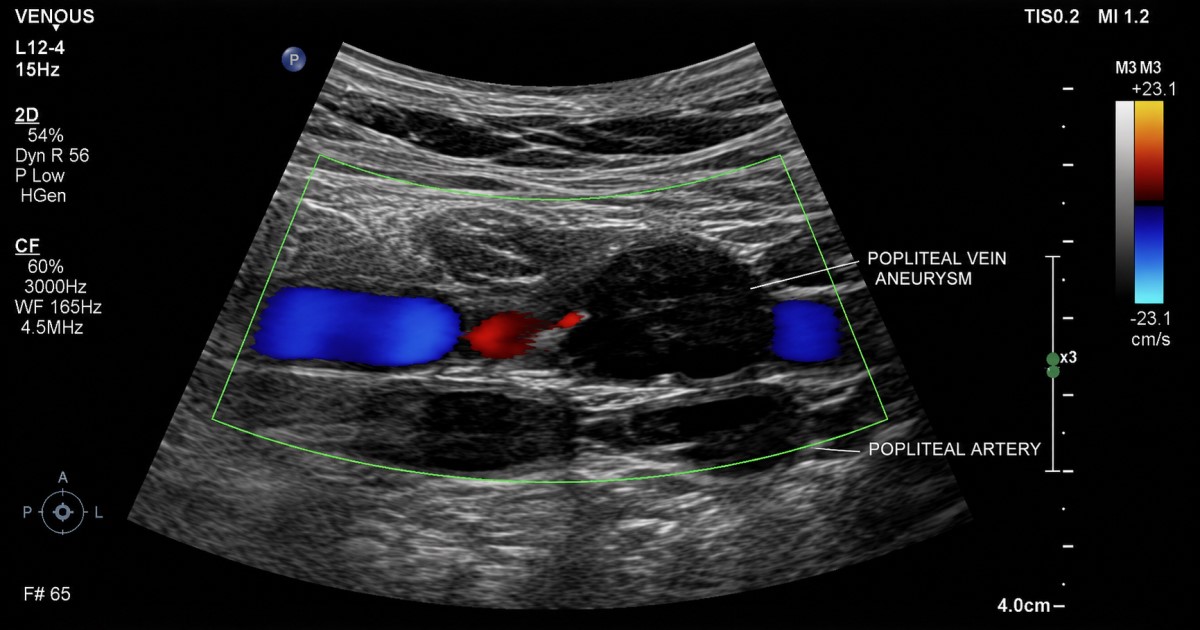
The evidence map treats diameter and morphology as practical decision signals, not just anatomy.
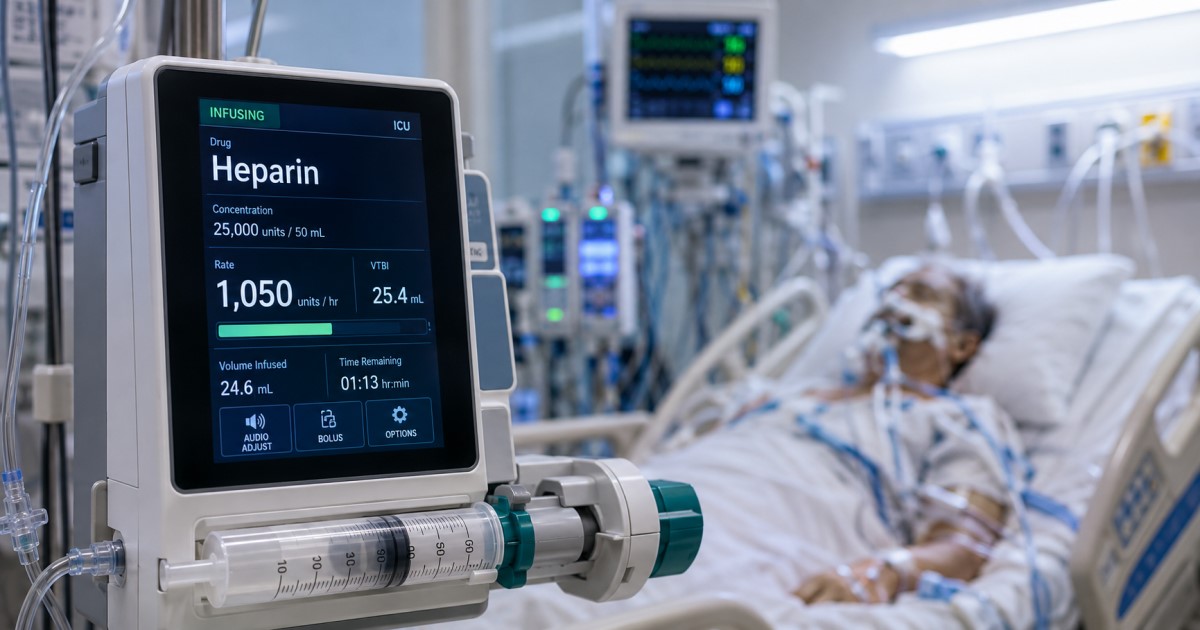
This is why symptomatic, thrombotic, large, or saccular PVAs often shift discussion toward repair and surveillance.
Unlock the full evidence map
The full evidence review, including the Introduction, Methods, Results, Discussion, Conclusion, figures, and complete reference index, opens after purchase or sign-in. The Evidence Object JSON is a separate machine-readable evidence product: a concentrated synthesis of results, topic-level evidence, and discussion across original and non-original studies. It can be directly input into your LLM, agent, or RAG workflow.